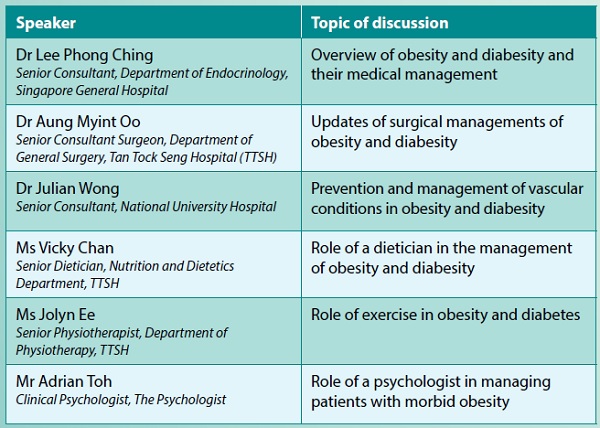
World Obesity Day is observed on 4 March and the theme for 2022 was "Everybody Needs to Act". In line with this, SMA organised a webinar titled "Fight Against Obesity and Diabesity" for primary healthcare professionals on 19 March 2022. The webinar was supported by Novo Nordisk and Bayer, and it drew a total of 176 participants. Speakers and the topics covered during the webinar are listed below. Also presented are some general information on the multidisciplinary management of obesity and diabesity for our fellow colleagues' reference.
Global twin epidemics
Obesity and diabetes are both global issues and they are widely regarded as twin epidemics worldwide. 800 million people around the world are living with obesity, and those with obesity are twice as likely to be hospitalised if they contracted COVID-19. Childhood obesity is expected to increase by 60% over the next decade, reaching 250 million by 2030.1 Worldwide obesity has nearly tripled since 1975, and most of the world': population live in countries where being overweight and obese kills more people than being underweight.2
537 million adults (one in ten) were living with diabetes in 2021. This number is expected to rise to 643 million by 2030 and 783 million by 2045. Almost one in two adults (44%) with diabetes remain undiagnosed (240 million). The majority have type 2 diabetes. 541 million adults are at increased risk of developing type 2 diabetes. Diabetes caused 6.7 million deaths in 2021 and was responsible for at least $966 billion in health expenditure in that year – 9% of the global total spent on healthcare.3,4 Obesity and diabetes are significantly linked to each other and thus the term diabesity (diabetes + obesity) was coined to correctly describe the metabolic syndromic effects of the combined health conditions.
The World Health Organization (WHO), as well as international medical and science societies have regarded obesity as a chronic progressive disease since 2013. Due to its progressive nature with high impacts on the well-being of both the individual and society, lifelong treatment and control is required for obesity.
Classes of obesity
According to WHO, overweight and obesity for adults are defined as follows:
Obesity and health impacts
People with obesity are at increased risks of various health conditions compared to those with a healthy weight. The risks include:
Obesity/diabesity management
The goal of therapy is to prevent and treat the obesity and its related complications and improve the quality of life. The goal can be achieved by a multidisciplinary approach including diet, exercise, behavioural therapy, pharmacotherapy and surgery. Health benefits have been reported with weight loss of as little as 5% body weight. With lifestyle measures alone, weight loss of 5% to 7% can be achieved; however it is often difficult to maintain in the long term. With the help of pharmacotherapy and behavioural modification, 5% to 10% of weight loss is considered a good response and more than 10% is an excellent response. Weight loss goals of 30% or more can only be achievable with the help of bariatric and metabolic surgery. For patients with diabesity, metabolic surgery can be considered for class 1 obesity patients with poor glycaemic control, in addition to lifestyle modification and pharmacotherapy.
Lifestyle modifications
Comprehensive lifestyle interventions with diet, exercise and behavioural therapy with the help of dieticians, physiotherapists and psychologists can help achieve 5% to 7% weight loss. The interventions include a balanced low-fat, hypocaloric diet and a minimum of 150 minutes of exercise per week (such as brisk walking). With the improvement of exercise tolerance over time, a multicomponent exercise training programme that includes aerobic and resistance training is preferred. With the help of behavioural therapy supported by clinical psychologists and clinical support groups, the goals can be easily achievable and sustainable.
Pharmacotherapy
Pharmacotherapy is an effective and helpful adjunct to comprehensive lifestyle modifications in obesity and diabesity management. Weight loss medications can be considered for selected patients with BMI >30 (27.5 for Asians), or BMI >27 (24.5 for Asians) with at least one obesity-related comorbidity, including type 2 diabetes. The decision to initiate pharmacotherapy is individualised after considering all the risks and benefits. Single agents are usually preferred over combination medications as initial therapy and for most patients, a glucagon-like peptide 1 (GLP-1) agonist (eg, Liraglutide or Semiglutide) is the preferred first-line pharmacotherapy in the treatment of obesity and diabesity.
Surgical management
Surgical intervention (eg, bariatric surgery for obesity, metabolic surgery for obesity with metabolic syndrome) can achieve as much as a 40% weight loss at 12 to 18 months postoperatively with long-term weight loss maintenance. In a joint statement by the International Diabetes Organisations published in 2016, metabolic surgery is recommended for class 3 obesity and class 2 obesity with poor glycaemic control while it is to be considered in class 2 obesity with adequate glycaemic control and class 1 obesity with poor glycaemic control.6 Bariatric/metabolic surgical procedures are either restrictive, malabsorptive or a combination of both. Most commonly done surgical procedures worldwide that are endorsed by the American Society for Metabolic and Bariatric Surgery are sleeve gastrectomy, Roux-en-Y gastric bypass, adjustable gastric band, biliopancreatic diversion with duodenal switch and single anastomosis duodenal-ileal bypass with sleeve gastrectomy.7 All surgical candidates are managed preoperatively and postoperatively by a multidisciplinary team comprising primary care physicians, bariatric physicians, surgeons, dieticians, physiotherapists and psychologists. With the help of the comprehensive multidisciplinary team approach, maintained weight loss with healthier lifestyle modifications can be successfully achieved.
Conclusion
Obesity and diabesity are chronic complex diseases and their prevalence is increasing yearly. As per this year's theme for World Obesity Day, let us act together hand in hand to fight against obesity and diabesity.
