To respect privacy and maintain confidentiality, all personal details of individuals mentioned in this article have been altered or anonymised.
My wife and I are doctors from Singapore and have been serving in Timor-Leste in the health non-governmental organisation (NGO) Maluk Timor for the past four years, We are supported by a diverse stream of short-term volunteers, usually young professionals from developed countries dipping their toes in global health work for the first time.
Below are seven recurring questions about volunteering that we often receive from prospective volunteers with Maluk Timor, along with our current thoughts and answers.
Will volunteering help me decide if global health is for me?
This often is the question. It drives many a young doctor to pack their bags, kiss goodbye to their loved ones and broadband Internet, and venture to a strange land. They are tempted by the prospect of going off the beaten career path, but uncertain if global health is truly their calling. They hope that their six months with us might reveal their fit; however, I try to temper expectations.
You know that story of the blind men studying the elephant, each arriving at a different mental picture of it after feeling a different part of its body? Welcome to the elephant's armpit. We are a small, unglamorous, slightly damp niche. Maluk Timor is an NGO in an underdeveloped, post-conflict country that is focused on strengthening the nation's healthcare system. We mainly train local doctors, nurses and midwives in primary healthcare.
There are many important aspects of global health work that we are not involved in. Serving with us will not give you familiarity with running a mobile clinic, engineering a water system for a village, negotiating food security with policy wonks, managing a refugee camp under artillery fire, or advancing vaccine research.
With that caveat, my answer to "Will volunteering help me decide if global health is for me?" is: "Sure!"
My wife and I have meandered into our current roles only thanks to 20 years of trial and error – and providence. Like many of our medical school friends, we started this journey through hesitant short-term commitments. These ranged from a classic three-day medical mission trip to Batam, Indonesia in 2002, to investing a year reestablishing a medical school in Sierra Leone after the Ebola outbreak of 2016.
How much time do I need to set aside?
The most common way we disappoint prospective volunteers is by turning away applicants who cannot commit to the mission for at least three months. This is painful to contemplate under the pressures of lost income and vanishing annual leave. There is of course a universe of worthy shorter-term opportunities just a couple of Google clicks away, but for our distinctive work, this length of time is the bare minimum for incoming visitors to simply settle down, get their bearings of the culture and language, and begin contributing.
This is a function of our peculiar type of work. Strengthening health systems, like fixing mechanical watches, is hard. The inputs are exacting, the work is delicate and our intermediate products are fragile. It becomes impossible to do if we are circulating new well-meaning volunteers on the work benches every few weeks.
It would be easier to welcome these short-term international volunteers into clinical work because healthcare delivery follows similar patterns, regardless of where you are. But fitting a volunteer into health systems work is a different matter altogether.
In our tuberculosis (TB) programme, for instance, we are focused on changing the national processes for household contact tracing in each newly diagnosed case of TB. This is a pressing issue as Timor-Leste has the second-highest TB mortality rate in the world. An incoming volunteer, regardless of his/her prior expertise in treating TB patients, must first figure out the jungle of national and international actors: front-line clinicians, health facilities, regional authorities, drug procurement bureaucrats, laboratory experts, Timorese Ministry of Health directors, technical advisors, international funders, etc. Just attempting to grasp who is who, the relationships and the unspoken rules can make you feel like you have been air-dropped into the middle of a Game of Thrones novel.
Thus, our response to "How much time do I need to set aside?" is: "At least three months."
What will be most difficult for me?
You will see awful things.
Many volunteers return home scarred by their intense experiences. One of my early encounters was when I cared for an eight-month-old child with meningitis, in a rural hospital in Kenya. We did not have the investigations, antibiotics or intensive care that he needed. My team understood he had been going downhill for 24 hours when he stopped breathing. As we started ventilations, I heard his mother, slouched in the far side of the room, whisper flatly, "He's going to die". She had already lost three children in the past five years. I paused, caught her eye and spat out, "No. He's not!" An hour later, we abandoned the resuscitation. I immediately shrank out of that room, unable to look at her again.
It is not the adverse patient outcomes alone that sting. Healthcare professionals – always, everywhere, unavoidably – are front-row audiences to suffering and death. Most of us build up emotional calluses. What slices through is bearing witness to unnecessary suffering. It is the moral distress of watching a tragedy which would have been unthinkable in better-resourced surroundings. That gnawing suspicion that it might have been averted if we had given just a little more, a little earlier. If we had been a little better.
My answer to "What will be most difficult for me?" is: "Witnessing unnecessary suffering."
I know of no salve for these wounds. I do not think we ever get over them. We just cry, pray and learn to live with them.
What skills should I pick up now to prepare myself for global health work?
We are most often asked this by students charting their journey of study and specialisation. It is an exceptionally difficult question to answer, because it depends on which of the myriad roles in global health you would like to end up in.
There are some broad competencies that would come in handy in most areas of global health work. My vote for the top three would be cultural competence, emotional resilience and broad academic disciplines such as public health, economics or management.
Then there is the specific technical domain expertise which varies depending on which bits of the elephant you attach yourself to. In this past year, I have found myself drawing upon lawyers (sorting out human resources policies), accountants (money is the lifeblood that keeps our NGO going), video editors (creating learning materials), data scientists (monitoring our programmes' performance), infectious disease physicians (redesigning our HIV services), and public policy experts (outlining health technology assessments).
Subjects I am currently studying include counselling (to better understand people affected by trauma), health informatics (to digitise clinical care delivery), and Bahasa Indonesia (to facilitate linkages with regional partners).
Thus, we respond to "What skills should I pick up now to prepare myself for global health work?" with: "Some general areas and some specific topics depending on the work."
What will everyday life be like?
The lifestyle you can expect ranges between the fixed poles of our most opulent donors to our most destitute beneficiaries. That can mean jarring transitions: sipping unpronounceable cocktails on a rooftop bar one night, then perching above an open pit latrine the next, swatting away Anopheles mosquitoes. Where on that spectrum will you spend most of your time? That is partly determined by your work and partly by your choices. Maintaining a lifestyle on par with back home puts you hopelessly out of touch with your immediate neighbours' realities, but trying to match theirs can create unsustainable stress.
My wife and I have opted for a spot near the middle of that curve. Our lifestyles in the field may be a notch below what we are used to in Singapore, but we are indisputably wealthy by Timorese standards, where over 40% of the population lives below the poverty line and half of all children are stunted from chronic malnutrition. Whenever we transition between home and the field, we are surprised by how malleable our sense of a "normal standard of living" is. After the culture shock wears off (probably about two to three months in), we will have recalibrated to our new milieu. Now, whenever visiting Singapore, I spend the first few days utterly astounded that I get to drink water right out of a tap!
Everything in daily life takes a little longer in a country that has not yet reached the machine-tooled efficiency of Singapore. This fact was especially impressed upon me after I undertook a four-hour quest, desperately searching every shop in the city for cat food.
But the most consequential difference is in the social and economic plumbing that lies beneath the veneer of daily life. The shaky infrastructure of public order, emergency services and medical evacuation generate an unceasing low hum of uncertainty, and that rises up through the humdrum. We are always on our guard, and our ears prick up at any news that around the corner is another riot, earthquake or cat food famine.
So, the answer to "What will everyday life be like?" is: "A wee less comfortable than you are right now... but you will get used to it. Mostly."
What are the people I will work with going to be like?
We work with numerous circles of people. The two that form the orbit of most international volunteers are our Timorese staff and other international volunteers.
The innermost circle comprises our 80 Timorese staff. They are alternatively sources of pride and paternal worry. We are regularly struck dumb by their personal stories of growing up during Timor-Leste's struggle for independence, their harsh early years and sometimes equally harsh present circumstances. They welcome international volunteers, are curious about their lives, and are hungry to learn from them.
The circle of other international volunteers is perhaps the most idiosyncratic. The global humanitarian sector is a self-selected gaggle of colourful characters, ranging from veritable saints to obnoxious ne'er-do-wells. There is a great number of PhD theses just waiting to be written somewhere, on the personality correlates of people who gravitate toward this chaos. Our first priority in processing volunteer applications is trying to filter out the weirdos (though we are not always successful).
The archetype that exasperates me most is what I call the "God's Gift". This is often a highly credentialed professional who descends upon the country for a couple of weeks with the presumption of prescribing cures, without deigning to understand our people or context. A close second is the "Activist", who is a rabid advocate for utopian solutions and packs a double helping of moral indignation for all who stand in their way. And third is the "Bleeder", whose bleeding heart compels him/her to race toward the centre of every perceived failure and tearfully render aid in a manner that cultivates dependence and eye-rolling.
What we say to "What are the people I will work with going to be like?" is: "Inspiring, unpredictable and eccentric."
What am I going to enjoy the most?
When departing volunteers tell us about what they enjoyed during the mission, the answers tend to converge on common themes: the sense of community (having neighbours' children named after you), quirky new experiences (riding in a minibus with a goat), and learning new skills (slaughtering the aforementioned goat for the baptism ceremony of the aforementioned child).
One sentiment often threads together their pre-trip hopes with their end-of-volunteering reflections: the awareness of having contributed to something meaningful. Health system strengthening work is hard, the gains are slow and the outcomes are brittle. Our horizons are years-long, so few short-term volunteers will see their individual effort bring about a major transformation. However, what they are privileged to see is constant forward motion. Project milestones ticking by. Our Timorese staff showcasing something they can do today that they would not have attempted yesterday. Patients receiving care that is a shade better than the week before. In a land where child mortality is 20 times that of Singapore, that drip-drip-drip of progress is water to one's soul.
Our answer to "What am I going to enjoy the most?" is thus: "Being a part of creating hope."

Oral health promotion in a village

Saying farewell to a departing volunteer
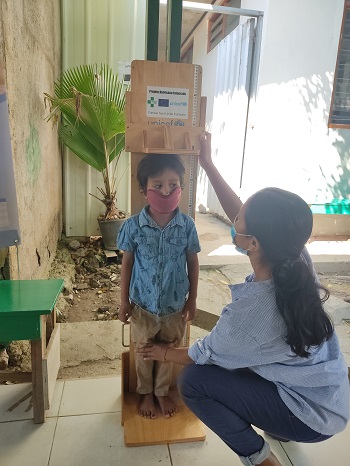
50% of all children in Timor-Leste are stunted
